This freaking sucks: fighting for in-network insurance coverage!
It sucks so bad…it will suck the life our of you. I have found myself in a new area of frustrations, one that is hard not trickle down into my family’s life. I knew it was coming, from the moment I signed that first paper…it kept popping back up and now it is becoming a reality.
I am so scared. I am so petrified. I fear for my family’s wellbeing. I am just scared.
As I log into the insurance portal, I see the massive amounts of dollars being attributed to George and Henry’s birth and stay at GHS’s NICU. Right now it is totaling around $260,000.00 for all the services and I am sure there are more to come.
The morning the twins were born was one of the biggest whirlwinds of my life. I had no idea which side was up or down. We were sent by Sarah’s OB with direct orders to bypass AnMed Health to go to GHS; Dr. Henry Hearn knew that if the twins were born at 32 weeks 5 days, they would have to go to the GHS’s Level 1 NICU.
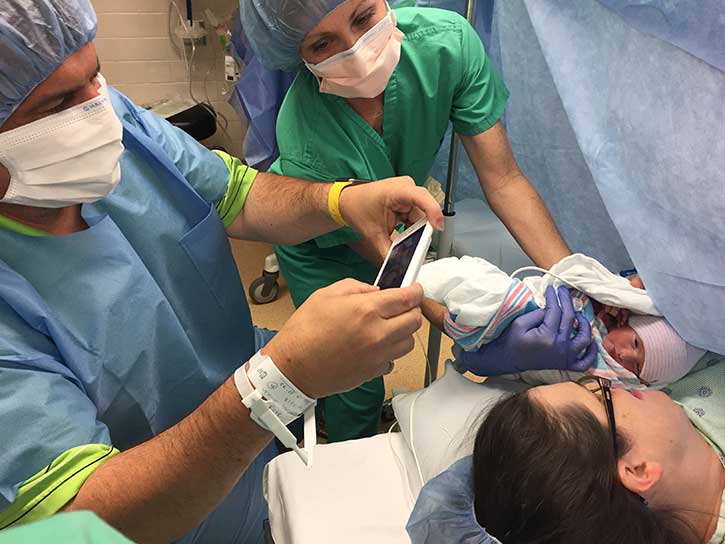
After the delivery, I followed the boys into the NICU. Tubes were being attached, people coming from all parts of the NICU to continue their initial assessment the boys, it was organized chaos, and I was trying to make sense of this developing normal. As I looked at my new baby boys, I see bubbles coming out of their mouth from the CPAP…I wondered, how did we get here yet excited to see them healthy and alive.
As I stood looking at my new family, so many people passing by, introducing themselves, explaining what is happening, and I was trying to make sense of it all. I was working off 2 hours of sleep and wish I had an audio recorder, someone collecting information for me, an assistant acting specifically on my behalf. I was wondering if I was gong to make the right decisions.
Then it happened, a lady asked me to sign a piece of paper, among many other pieces of paper. I had only been standing in the NICU for five minutes after the twins were born, it was time to sign papers.
- Release forms
- Patient information forms
- Lewis Blackman form
- A form to appeal to insurance that Pediatric Obstetrix should be considered In-Network
But this one was crucial and I did not realize how crucial it was until now. The lady, whom I do not remember her name, asked me to sign a piece of paper asking to appeal our insurance’s out-of-network policy for the physicians that work in the NICU at GHS to be considered in-network. She explained the importance and then explained they that these physicians are the only physicians in the region to provide this level of care.
This moment happened amongst all the other moments during that morning of June 10, 2017 and now I wish I could hit the rewind button.
Fast forward and now I am receiving claims letters showing that the physicians’s billing is not covered. These are the physicians that provided all the care for George and Henry from the moment they were born until the moment they were discharged 28 days later. These are the physicians of Pediatric Obstetrix, physicians with privileges at GHS Children’s Hospital. These claim amounts are now totaling around $60,000.00 and I could be responsible for these charges.
At 3:30am on June 10, 2017, I had no idea that I should ask Dr. Henry Hearn if we should go to GHS because the physicians might not be considered in-network. I had no opportunity while Sarah was bleeding really bad during that 30 minute drive to GHS if the physicians in the NICU were in-network? I did not even know if we would go to a NICU? How do I plan for in-network physicians for a NICU during an emergency? All I know…I was told by Sarah’s OB was to go to GHS immediately!
WHO HAS $60,000.00 LAYING AROUND????
As I begin to start my plan, I wonder…what if I cannot appeal this unknown situation? How will I come up with $60,000.00 to pay for the tremendous care provided for the twins.
I spend lots of money each month for insurance through UnitedHealthcare. I work in healthcare. I am surrounded each day with my healthcare clients. Yet, I cannot figure how this happened, being caught in a place where there is a looming $60,000.00 price tag on services that might not be covered.
As a single income family of five, that number can be a devastating number. As I begin to research, log into GHS’s and AnMed’s MyChart to pull transcripts of dictations to show we had no choice, no option, no idea…that this emergency situation with Sarah’s placental previa would take us to a place where the hospital is considered in-network yet the physicians that provide the care are considered out-of-network.
Devastating anticipation for this family…that is trying to put the focus on family, not the looming insurance uncertainty.


Yup. My wife has Medicare, but I’m still an “Individual”. This is a dirty word to most all healthcare providers. I don’t blame them, as it means hours on the phone with BCBS arguing about the silliest things. It means home in Texas there was ONE PROVIDER who would take new patients and be my PCP within 50 miles. It means that nearly every medical procedure happens after weeks or months of talking, writing, phoning and arguing.
We elected a bunch of people who said they’d rid us of ACA, and they are not. I’m seriously worried that this country I love is going to blow up — civil war, riots, terrorism — because of so many basic problems.
This is terrifying and ridiculous! Keep fighting and keep in their
ears! And I know i don’t need to tell you this, but if you all need
anything, let us know how we can help. (Also, just an aside and I know
you know this too, but it isn’t an ACA issue specifically, network
exclusion/deductibles/copays etc are long term issues associated with
rising healthcare costs over the past few decades and the structure of
insurance networks in the US. We had these same issues with my dad’s
surgeries in the 90s and 2000s and I had them when I had both my kids,
though not to the tune of $60k. Look over those bills with a magnifying
glass too, I discovered on the anesthesiology bill that I as being
charged for a C section I didn’t even have!)
You KNOW health care providers. You KNOW they care and want to provide the best care possible. Your doctors did not invent the networks. Nurses did not beg for restrictions on their ability to deliver care. The problems with the system are ALL built into the idea that INSURANCE is the basis for care and GOVERNMENT REGULATION is a better foundation for health care decisions than patient needs. Since the early 1960’s, with supposedly the best of intentions, government and insurers have put medical community intelligence and doctor/patient relationships far down the list of priorities as they designed a system that was supposed to be more equitable. They have created an alphabet soup of DRGs and PROPACS, PROs and HIIPA, to dictate FINANCIAL categories of diagnoses and create documentation accountability that has added cost, time, and a political component to health care — with process and compliance made far more important than patient well-being and treatment results. They have created a system in which doctors are at risk (defensive medicine) and lawyers and insurers have a louder voice than clinicians in the who/why/where.how of patient care. It is easy for people to say the “health care system” is broken — but it’s not quite accurate. FAR closer to the truth is that the health CARE system has been restricted in its ability to deliver quality care and had another system — one with networks and paper trails and insurers and legalese — put in its place. Neither medical professionals nor hospitals, nor even big pharma, are to blame for insane costs, diminished care, and expanded irrelevant process — THOSE daunting realities are the gifts of government.